Author: Dr. Deeik
The Beat Goes On
 To look at Clarence “Ed” Logan, you’d have a hard time believing the man is 80 years old, much less that he recently went through valve replacement surgery. The spry Fairfield resident loves to spend time with his bride of 55 years, Maureen, and take walks with his spunky Jack Russell terriers, Tugg and Buddy.
To look at Clarence “Ed” Logan, you’d have a hard time believing the man is 80 years old, much less that he recently went through valve replacement surgery. The spry Fairfield resident loves to spend time with his bride of 55 years, Maureen, and take walks with his spunky Jack Russell terriers, Tugg and Buddy.
But it was on one of those walks when he realized something was not quite right. Out of the blue, he was having a hard time breathing.Ed, who retired from the Air Force and then from the City of Fairfield after 20 years, has always been active, cutting wood, doing chores, taking long walks. He’d had a heart attack when he was 51, and so he knew what he had to do to take care of himself.
With a family history of heart issues, he stayed in contact with his cardiologist, who was keeping a watchful eye on his aortic valve. Suddenly, he was a good candidate for a valve replacement.
No longer do patients like Ed have to travel outside Solano County for such a procedure. NorthBay Healthcare opened its Heart & Vascular Program in April 2009. At the time, valves weren’t really part of the plan. “We were anticipating bypasses, mainly,” explains Acute Care Nurse Practitioner Jamie Wheelahan. But only a few months later, valve surgery became a reality at NorthBay, and has been ever since.
“We realized rather quickly that we had everything we needed to do valve surgery,” says Ed’s surgeon, Ramzi Deeik, M.D., director of Cardiac Surgery at NorthBay Medical Center. “Our operating room is state-of-the-art and not short in any way of the latest and greatest technology. That allows complicated surgeries such as valve replacement to go smoothly.”
Still, the procedure is no walk in the park. In order to replace or repair a valve, the heart has to be completely stopped.
The Medtronic Performer, a state-of-the-art heart and lung machine, pumps blood through the body and is maintained by a top-notch perfusion team, says Dr. Deeik. The equipment is completely computerized and follows the values of patient temperatures, electrolytes and even features bioactive coating on its tubes, which prevents clotting. “That means we can use less blood thinner during the surgery.”
For many patients, blood thinner is part of their reality after valve surgery. That is, if they decide to have a mechanical valve. After consulting with Dr. Deeik, it was determined that Ed would be given a tissue, or porcine, valve so he won’t have to be on the blood thinner Coumadin the rest of his life. “There’s less stress. They don’t have to worry about using too much or too little. And a tissue valve, especially in an older person, can last up to 25 years,” says Dr. Deeik.
Ed’s surgery took a little over two hours. “We are very expeditious,” recalls Dr. Deeik. “We don’t want to keep the heart arrested for a long period of time. The national average is 90 minutes, but mine is usually less than an hour.”
Dr. Deeik says he doesn’t hesitate to replace the valve of a patient who is in their 80s or even 90s.
“Look at the alternative,” he says. “They have a tight valve that doesn’t allow blood to leave the heart, they’re not getting enough to the brain, their arms or legs; they feel tired and weak, their body is hungry for oxygen and blood. The heart is working overtime to squeeze blood out of a tiny hole.” When a heart works that hard—sometimes for years—it ultimately will start failing. Although the recovery process was a little rough, Ed’s feeling “really good now,” he says. He goes to NorthBay’s cardiac rehab program three times a week, and is back to walking his beloved dogs. They bicker at his feet over a new toy Maureen made using Ed’s hospital stockings and a couple of tennis balls.
“I can’t believe how much help I got from all the staff there, especially in the ICU,” Ed recalls. “Everybody was great, very compassionate.” Even after he was home, NorthBay Health at Home took some of the burden off, by installing a computer in their bedroom, checking on his vitals and staying in close contact with Ed and Maureen.
“It was really good help,” says Maureen, who confides that at one time she wanted to be a nurse. She got her wish, helping Ed navigate those first scary weeks. Now the couple is planning a trip to Hawaii to celebrate.
It’s just another success story for Dr. Deeik, hailed in the industry as “the Valve Surgeon,” because it has become his specialty. He frequently gets referrals from other hospitals in the region.
New Hope for Young Hearts
Go Red for Women Event • American Heart Association
Michelle and I attended a wonderful event on Friday, May 7, 2010. It was the Go Red for Women Event. The event was organized by the American Heart Association and the event was made possible by a large number of local sponsors.
The message was very clear:
- Take Charge of Your Own Health – Visit your Doctor, know your numbers and work toward improving your blood pressure, cholesterol and other numbers by making life style changes.
- Speak Up – Spread the word, Heart Disease is women’s #1 Killer.
- Consider Making a Donation – Your donation will help fund local and national Go Red activities to support awareness, research, education and community programs to benefit women.
The symposium featured the following speakers:
- Ari Hauptman, M.D., F.A.A.P. with the Department of Pediatrics at Kaiser Permanente – Dr Hauptman spoke to us about childhood obesity. He had suggestions on How to Prevent and Treat Childhood Obesity.
- Rami Turk, M.D., Medical Director of the Vascular Department at Northern Californian Medical Associates. Dr. Turk talked to us about Heart Disease being women’s number 1 killer and what we can do about it.
- Ramzi Deeik, M.D., Director Cardiac Surgery, Santa Rosa Memorial Hospital & Cardiac Surgeon at the Queen of the Valley Medical Center. Dr. Deeik spoke about the advances in Cardiovascular Surgery.
At lunch, we had a Heart Healthy lunch…beautiful salad and dessert provided by the Hyatt Vineyard Creek (the location of the event). During lunch we heard from Mrs. Condoni. She talked about Joey, her 7 year old son. He was born with half a heart. At 7 years old, he has survived three surgeries and continues to inspire people around him with his courage. She made a very heart felt plea for donations to the American Heart Association. Santa Rosa Firemen passed out a RED boa to everyone that made a commitment on the spot.
The key note speaker was Kirk Papas, M.D. He is a Physical and Rehabilitation Doctor at Permanente Medical Group at Kaiser Santa Rosa. He talked about the importance of moving your body. He talked about committing to 150. (Our interpretation; he wants us to commit to 150 minutes of aerobic exercises a week…this would be about 20 minutes per day.)
At the conclusion, there was a Live Auction and Fashion Show.
It was a wonderful event and it was for a good cause. We encourage everyone to consider giving a donation to the American Heart Association (see the link below). And, attending next year’s event.
Surgical Team focuses on Heart of the Matter
 NorthBay Medical Center’s unique situation and location will make it one of the most sought-after heart programs in Northern California, says Dr. Ramzi Deeik, director of Cardiac Surgery Clinical Outcomes at the NorthBay Heart & Vascular Center. The cardiothoracic surgeon has been with the program since its planning stages.
NorthBay Medical Center’s unique situation and location will make it one of the most sought-after heart programs in Northern California, says Dr. Ramzi Deeik, director of Cardiac Surgery Clinical Outcomes at the NorthBay Heart & Vascular Center. The cardiothoracic surgeon has been with the program since its planning stages.
It has taken two years, lots of planning and millions of dollars in equipment, training and recruiting, but today NorthBay Medical Center has a five-man surgical team ready to take on heart, vascular and thoracic cases in its new state-of-the-art surgical suite. Now patients can come to the Fairfield facility for everything from open heart surgery to valve repair.
“It’s been an honor to be involved in the initial stages of developing this heart program,” says Dr. Deeik. The planning committee began nearly three years ago, and was made up of physicians, administrators, experts in the field, nurse practitioners and leaders throughout NorthBay Healthcare. “It’s been a very unique experience,” says Dr. Deeik. “We have a very dedicated team of people here who are excited about what they’re doing.”
While the surgery team has had plenty of experience at other Northern California hospitals, that was not the case for others on the team. Before the first surgery could take place in Fairfield, NorthBay nurses had to go to other hospitals for hundreds of hours of training.
“The nursing staff’s new expertise was really on display when the first surgery was performed,” recalls Dr. Deeik. “The feelings we shared during that first operation back in April were incredible. The fact that we were able to help patients in their own community and make sure their family was close to home, well, patients do extremely well in the recovery process. It has been very uplifting.”
https://wellspring.northbay.org/surgical-team-focuses-on-heart-of-the-matter/
Bypass Surgery ~ A Success Story: Norman’s Journey
 When it comes to matters of the heart, everyone’s experience is different. Some stroll into the Emergency Department with “a little indigestion” and shortness of breath, while others are rushed in on a gurney suffering cardiac arrest.
When it comes to matters of the heart, everyone’s experience is different. Some stroll into the Emergency Department with “a little indigestion” and shortness of breath, while others are rushed in on a gurney suffering cardiac arrest.
In some cases, a simple stress test can start the journey, which could lead to an interventional procedure or open heart bypass surgery. Response and treatments are as diverse as the patients themselves.
Still, NorthBay Medical Center – now a recognized national Chest Pain Center – has established rigorous standards and best practices in dealing with heart patients.
And while no two patients are exactly alike, each case is similar in several ways. To help potential patients, their families and friends understand the ins and outs of cardiac care, Wellspring was invited to tag along with Fairfield residents Norman Gray and his wife, Jackie. As you read how his heart started to heal after a triple-bypass, beating heart surgery in May 2009, you will be introduced to the teams that comprise the heart of NorthBay’s Heart & Vascular Center.
His triple bypass surgery was just the beginning
The night of May 15, 2009, is still a blur to Norman Gray.
The 66-year-old retired assistant truck stop manager was trying to sleep, but something was wrong. Five months earlier he had undergone an interventional procedure that placed two metal stents (tiny tubes of wire mesh) in arteries around his heart to open a blockage.
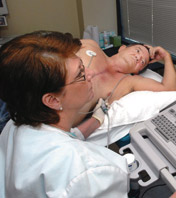
Things seemed to be going well, until that night. He was restless, and couldn’t seem to get comfortable. When his labored breathing became gasps for air, his wife Jackie dialed 911.
The Grays spent 12 hours in the Emergency Department that night. Norman remembers little of it, and Jackie remembers all too much. There was the ride in the ambulance, a seemingly endless number of tests and a visit to the cardiac catheterization lab for an angiogram, which helped determine that Norman was going to need surgery: a triple bypass.
Norman had had a heart attack.
Surgery became necessary. After waiting several days in intensive care for the blood thinners he had been given in the Emergency Department to wear off, things moved quickly.
Remembers Jackie, “People started coming out of the walls. The whole program starting clicking right then.”
That’s when the Grays met Acute Care Nurse Practitioner Jamie Chohon and ICU nurse Paula Azure, R.N., who Norman calls his guardian angels. Norman’s appointed surgeon, Dr. Ramzi Deeik, director of Cardiac Surgery at NorthBay, came by to visit and explain what was going to happen.
“His heart was working at about 50 percent of capacity,” recalls Dr. Deeik. “That means his heart muscle was thirsty for more blood flow and oxygen. The beating heart surgery allows us to operate on the heart while it’s beating. We don’t need to stop it, or arrest the heart. By doing so, the heart will tolerate the operation better. There is less risk for bleeding and blood transfusions, kidney failure or lung problems.” It meant the best chance for a quick recovery and fewer complications for Norman.
The Grays were given NorthBay’s “Cardiac Surgery: Patient & Family Handbook,” which Jackie calls her ultimate guide to navigating the journey. Jackie says on Monday she started to recognize people from the book. Several pictured in it came by to introduce themselves and to patiently answer all the questions the Grays and their family had.
Norman remembers going from Room 21 to the elevator on the day of surgery.
They put an IV in, and “the rest is history,” he chuckles.

“History” actually involved a four-hour surgery, and six days in ICU before being discharged.
Veins had been harvested by a scope from Norman’s legs, leaving inch-and-a-half-long incisions, which healed quickly.
The recovery team at NorthBay included physical and cardiac rehabilitation therapists and a nutritionist, all devoted to making sure the Grays would be comfortable and confident to continue the healing process at home.
Norman learned how to safely get in and out of bed, using a pillow to brace against his healing breast bone. He was given post-surgical exercises to help him build his strength. And a nutritionist helped him determine the right combination of medicines and diet to stabilize his blood sugar and blood pressure.
“Discharge planning starts from the moment the patient comes through the doorway,” explains Tina Simon, R.N., inpatient case manager and discharge planner.
“I was involved in Norman’s journey from the beginning. I followed his pathway from hospitalization through discharge, maintaining contact with patient, family and staff and coordinating his discharge care.”
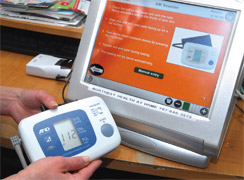 Norman was finally released with supervision from NorthBay Health at Home.
Norman was finally released with supervision from NorthBay Health at Home.
This is a program that allows a patient to recover at home, but under the watchful care of a medical team. It was decided that a Telehealth monitor could be installed in the Grays’ bright-green mobile home in Fairfield. Each day, Norman had to answer questions on the computer screen. It helped him track his vitals. “Blood pressure, blood sugar, weight, everything,” says Jackie, noting it was a huge relief.
“All that information went directly to the nurses and doctors. They were in constant contact,” she says. “That eases the caregiver’s mind a lot.”
Of course, once Norman was on the mend, the monitor was removed.
He began a rigorous schedule of checking in with his primary doctors, including his endo-crinologist, and his cardiologist.
A July visit with his endocrinologist Dr. Deborah Murray left the Grays overjoyed. Despite a shaky start maintaining his blood sugar, Norman managed to get his average glucose (or hemo-globia A1c) levels down.
“This is perfect,” an enthusiastic Dr. Murray told the couple. “This is almost non-diabetic.
It means that you’ve made such a change in your blood sugars that you’re almost normal. This is remarkable.”
Norman was diagnosed with type 2 diabetes in 1998. Maintaining his blood sugar had always been a struggle, Jackie recalled.
The heart attack was a wake-up call that couldn’t be ignored.
“Heart disease is the thing that kills diabetics,” explains Dr. Murray. “Eye disease, kidney disease, vascular disease and amputations are all things that people think about that are complications of diabetes which we try to avoid. Those are terrible, but what kills the diabetic is cardiovascular disease.”

The Grays then met as a team with Norman’s cardiologist, Dr. Milind Dhond, who was pleased with his progress. He took note of his medications, checking on the cardiac rehab schedule and scheduling a followup echocardiogram to stay on top of Norman’s progress.
“While a patient might meet once with their surgeon before, and once after a procedure, they’ll usually never see the surgeon again,” explained Dr. Dhond. “But the relationship with their cardiologist becomes a lifelong thing for the patient. It is the modification of risk factors, leading a healthy life, keeping weight issues under control, and doing all those things.
If all goes well, we’ll be seeing each other for many years to come.”
In cardiac rehabilitation three days a week at NorthBay Medical Center for a 12-week stint, Norman attacks the bikes and the treadmill with gusto.
His every action is closely tracked. He wears a monitor that reports his blood pressure, pulse and other key stats to nurses who run the facility.
It’s a mini-gym of sorts, with exercise equipment squeezed into a main room ringed by offices. “They work you good,” Norman confides between exercises.
The women who oversee the operation have all been intensive care nurses with cardiac experience.
“I know I can go to work and he can go to rehab, and he’ll be in good hands,” says Jackie.

Debbie Gordon, clinical manager of NorthBay Cardiac and Pulmonary Rehabilitation, confirmed that Norman was right on track, learning to manage his routine, his blood sugars, his diet and exercise.
Several months later, Norman’s rehab gym time is over, but his exercise routine continues.
He walks nearly every night with Jackie, and works out every day at a local gym. He has lost 20 pounds since his surgery and established a whole new diet and exercise routine. He has also gained a healthy new outlook on life.
The journey, say the Grays, would not have been possible without a dedicated team at NorthBay Medical Center that has continued to check in with the couple over the past several months.
During a recent hospital visit, Norman took his “NorthBay” bright red, heart-shaped pillow and asked “his heart team” to autograph it. It sits on a special shelf in his living room, a reminder of how many people literally and figuratively touched his heart.
Cardiac Surgery Has Successful Start
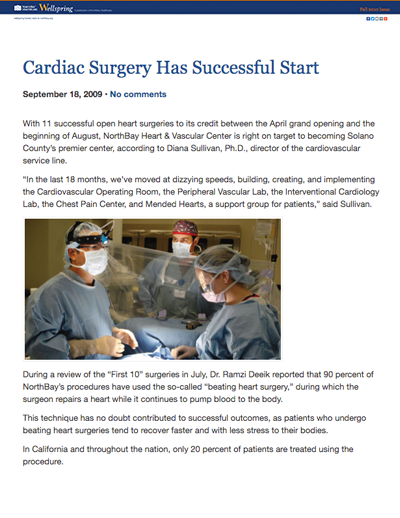 With 11 successful open heart surgeries to its credit between the April grand opening and the beginning of August, NorthBay Heart & Vascular Center is right on target to becoming Solano County’s premier center, according to Diana Sullivan, Ph.D., director of the cardiovascular service line.
With 11 successful open heart surgeries to its credit between the April grand opening and the beginning of August, NorthBay Heart & Vascular Center is right on target to becoming Solano County’s premier center, according to Diana Sullivan, Ph.D., director of the cardiovascular service line.
“In the last 18 months, we’ve moved at dizzying speeds, building, creating, and implementing the Cardiovascular Operating Room, the Peripheral Vascular Lab, the Interventional Cardiology Lab, the Chest Pain Center, and Mended Hearts, a support group for patients,” said Sullivan.
During a review of the “First 10” surgeries in July, Dr. Ramzi Deeik reported that 90 percent of NorthBay’s procedures have used the so-called “beating heart surgery,” during which the surgeon repairs a heart while it continues to pump blood to the body.
This technique has no doubt contributed to successful outcomes, as patients who undergo beating heart surgeries tend to recover faster and with less stress to their bodies.
In California and throughout the nation, only 20 percent of patients are treated using the procedure.
In addition to nine off-pump surgeries, and one traditional coronary artery bypass surgery, NorthBay’s team also performed a valve replacement surgery.
“The project development is the culmination of the 20-year vision of Gary Passama, NorthBay Healthcare president/CEO with the supportive leadership of Chief Nursing Officer Kathy Richerson and unprecedented teamwork of the hospital management,” said Sullivan.
“There is a lot of excitement, and a nice thing that I see when I come to the hospital is how the nurses’ faces are all glowing, they are so proud to take care of heart patients,” said Dr. Deeik during a summer service line meeting.
NorthBay Medical Center has dedicated a room, located near the front lobby, for families and friends of heart and vascular patients. The room, formerly a meditation area, has been set up to be a private, comfortable suite where the family can watch television or rest while waiting for their loved one.
http://wellspring.northbay.org/articles/cardiac-surgery-has-successful-start
Open Heart Surgery Debuts
 “…as Americans get more obese and live longer, heart surgeries are increasing.
“…as Americans get more obese and live longer, heart surgeries are increasing.
‘As you get older, all the things that take your life present themselves.’
The surgeons said they will use an ‘off the pump’ style of operating. That means the heart will continue to beat during the open heart surgery, instead of hooking a patient up to a machine.
Along with the heart surgery, the surgeons said they were looking forward to the possibility of eventually performing vascular surgery for patients with lung cancer.”
At Queen of the Valley, doctors back away from patient to guide a robot that performs open heart surgery
 “The Queen uses a robot, controlled by a surgeon seated at a panel across the operating room from the patient, to offer a minimally invasive alternative.
“The Queen uses a robot, controlled by a surgeon seated at a panel across the operating room from the patient, to offer a minimally invasive alternative.
Patients such as Straus and Bajakian are back on their feet within a day.
Straus was sent home from the hospital in less than two days. Bajakian was back home 24 hours after her surgery.
Dr. Ramzi Deeik performed both robot-assisted surgeries.
“Our emphasis is on minimum patient trauma,” the veteran heart surgeon said. ‘The robot allows us to do that.'”
ESTECH Beating Heart Surgery Devices Achieve Key Milestone
 “Ramzi Deeik, M.D. of Queen of the Valley Hospital at Napa Valley Medical Center in Napa, Calif., was the first surgeon in the San Francisco Bay Area to perform the ESTECH-style procedure, on an 86-year-old patient.
“Ramzi Deeik, M.D. of Queen of the Valley Hospital at Napa Valley Medical Center in Napa, Calif., was the first surgeon in the San Francisco Bay Area to perform the ESTECH-style procedure, on an 86-year-old patient.
Dr. Deeik used the Da Vinci Robot by Intuitive Surgical, Inc. to isolate the left internal mammary artery for use as a bypass graft through three 10-millimeter ports. The ESTECH Access and Stabilization System were inserted into another small incision, or “window”, between the ribs, allowing him to bypass a blockage in the left anterior descending (LAD) coronary artery without stopping the heart.
Commenting on the procedure, Dr. Deeik said, “ESTECH technology that allows surgeons to perform heart surgery on a beating heart through a two-inch incision provides great benefits to patients, reducing complications and recovery times.”
